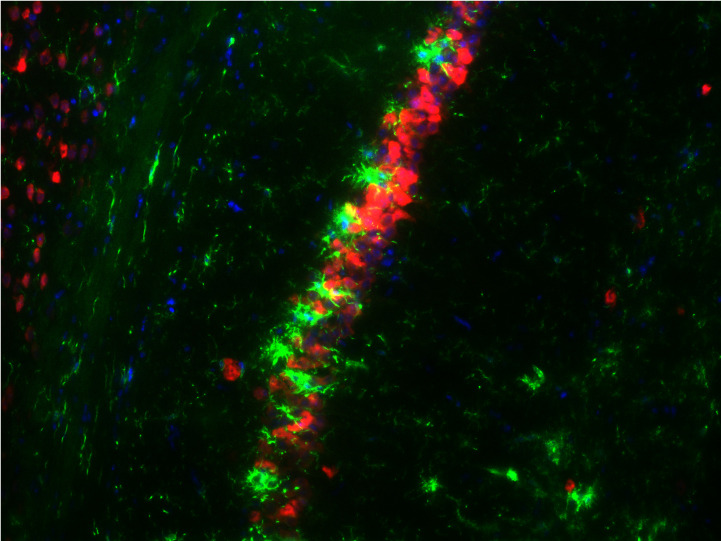
This image depicts a section of a brain a week after an initial seizure. In such cases, microglial cells, stained green, sometimes engulf and attack neurons, stained red. Two drugs currently being tested in an ISU biomedical sciences lab may silence or control the microglial cells and prevent spontaneous seizures. Photo courtesy of Thimmasettappa Thippeswamy. Larger image.
AMES, Iowa – Ongoing research at Iowa State University is investigating the connection between initial seizures and the onset of epilepsy later in life.
Nearly one in 10 Americans will experience an initial seizure, but only 3 percent of those who experience a seizure will go on to develop epilepsy, according to the Centers for Disease Control and Prevention. Thimmasettappa Thippeswamy, a professor of biomedical sciences in the ISU College of Veterinary Medicine, is studying why some who suffer a seizure develop the disease and others don’t.
A related question Thippeswamy is investigating is why a small fraction that develops the disorder doesn’t respond to the most common drug treatments for epilepsy.
Thippeswamy said medical science has a poor understanding of why only some people who have a seizure develop epilepsy – sometimes years after the initial seizure – and why conventional medications don’t always help.
His lab members are tracking long-term brain activity in rodents after experimentally induced seizures. They’re looking closely at how two experimental drugs work in concert with one another to gain a better understanding of epileptogensis, or the process that leads to the development of epilepsy. Thippeswamy said gaining a better understanding of epileptogensis may hold the key to halting the progression of the disease.
They’re using radiotelemetry to study effects of the drugs in real time. The research has offered new insight into how seizures affect the behavior of neurons and glial cells, critical brain cells that process and relay information, in the parts of the brain that govern learning and memory.
Thippeswamy said seizures can stimulate the birth of new neurons, but the new cells don’t always integrate well with the existing neurons. The two drugs Thippeswamy is studying may be able to make the transition easier for new neurons.
“When neurons don’t work in a coordinated manner after the first seizure, they send a ‘wrong message’ to the glial cells,” Thippeswamy said. “The glial cells will turn into bad guys, and may pick on bystanders such as newborn neurons. We’re investigating whether the drugs can turn these bad guys into good guys.”
He also said antioxidants, such as those found in natural food products like grapes or greens, may act in a similar way as the experimental drugs, since some antioxidants affect the same targets in the brain.
Thippeswamy said his research also has implications beyond classical epilepsy; for example, he said it could impact those who suffer from traumatic brain injuries, such as veterans or athletes competing in contact sports.