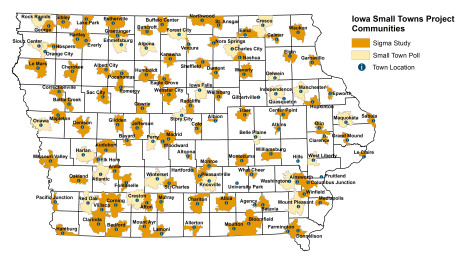
AMES, Iowa – More than a million Iowans are at an increased risk of dying from heart disease, cancer or a stroke simply because they live in a rural area.
Higher rates of smoking, high blood pressure and obesity among rural Americans, as well as poverty rates and access to health care all contribute to this disparity, according to the Centers for Disease Control and Prevention. National Rural Health Day on Nov. 16 aims to reduce the gap in rural and urban health outcomes – something Iowa State University researchers are directly and indirectly doing through their research and ISU Extension and Outreach initiatives.
Sarah Francis, associate professor of food science and human nutrition and extension specialist
Proper nutrition and exercise are necessary for good health, regardless of where you live. Unfortunately, going to a gym or even having a grocery store with healthful foods nearby is not an option in many rural areas. Recognizing these challenges, Francis and colleagues have designed and implemented programs to promote health and wellness.
Latinos Living Well, which offers classes on nutrition and physical activity with the goal of preventing the onset of Type 2 diabetes, is one of her most recent efforts. Latinos are twice as likely to develop diabetes, but many do not know if they have the illness or may be at risk, Francis said. The risk combined with the growing Latino population in rural Iowa has created a need for these culturally appropriate classes (taught in Spanish) to help Latinos develop healthful lifestyles. Data collected during a pilot of the Latinos Living Well program found participants grew more confident about managing diabetes through lifestyle changes, exercised more and prepared class recipes at home.
“As the Latino population grows, we must respond with culturally appropriate, impactful programming,” Francis said. “The program is research-based, which is especially important in rural areas where limited health care access and fewer physical activity opportunities may exacerbate diabetes risk.”
Francis and a team of Extension nutrition and wellness specialists across the state also offer a Wellness and Independence through Nutrition program. The goal is to improve nutrition and quality of life for older adults by helping those who are eligible be more aware of the Supplemental and Nutrition Assistance Program. Since 2014, more than 4,500 older adults have participated and 117 were referred to the Food Bank of the Heartland for application assistance.
Kimberly Greder, associate professor of human development and family studies and extension specialist
Access to mental health services is not the only barrier for people living in rural communities. Greder says cost and distance often prevent people from seeking help, but stigma is also a problem. Much of her research focuses on the mental and physical health of low-income families in rural communities. Even if families have the resources for treatment, she says they are often ashamed or embarrassed.
“In a town of 10,000 residents, everyone is going to know if your car is parked outside the therapist’s office,” Greder said. “The tight, close-knit aspect of rural communities is a great thing, but it also makes it difficult to ask a friend or neighbor for help, especially if it’s related to a mental or emotional issue. We need to help families realize it is OK to seek help or talk with others when they’re not feeling well mentally.”
Children participate in a Zumba class as part of the Abriendo Caminos program in Perry. Photo courtesy of Kimberly Greder
Improving physical health can also benefit mental health. Through her extension efforts, Greder coordinates the Abriendo Caminos program for Latino families in Perry, Postville and Ottumwa. Over the course of six weeks, parents and children learn about nutrition and physical activity, and work together as a family to make decisions and set goals on how to live a more healthful lifestyle. Greder is working with researchers at the University of Illinois to collect data and evaluate the program.
There is also a misconception that families in rural communities have ample access to outdoor space for physical activity, Greder said. However, her research has found the green space is not always usable or convenient. Low-income, rural mothers interviewed for the study reported they did not have access to parks with age-appropriate equipment or safe walking trails.
Jennifer Margrett, associate professor of human development and family studies
With a growing number of older adults in Iowa, many living in rural areas, Margrett is concerned about the lack of qualified workers, support services and care facilities for people with dementia. She and her colleagues are working on solutions to improve health care access in counties labeled “care deserts” or classified by the CDC as medically underserved.
Nearly 80 percent of Iowa counties have segments of the population that are medically underserved, which affects all aspects of the life span from infant mortality to care for older adults who want to age in place, Margrett said. In a medical emergency, people living in these “care deserts” are miles away from the closest hospital, which might not have specialized care. Margrett says they may delay or not seek treatment for mental health or preventative care because distance is a barrier.
“Our data also looked at whether adults had someone they could turn to if they needed help. A high number of Iowans in rural areas felt they had no one they could rely on,” Margrett said. “The concern in these care deserts is not just formal support, such as doctors and specialists, but also informal support from family, friends and neighbors.”
Christopher J. Seeger, professor of landscape architecture and extension specialist
Creating walkable, pedestrian-friendly communities and landscapes provides safe routes for children walking or biking to school and an avenue for older adults to increase their physical activity. Seeger, in partnership with the Iowa Department of Public Health, has worked with 50 Iowa communities to tackle this issue through the I-WALK (Iowans Walking Assessment Logistics Kit) project. The main goal was to identify infrastructure gaps where communities need to extend sidewalks or address other problems.
Seeger and colleagues with Iowa State Extension and Outreach are building upon that work to provide city and county governments or agencies with data to improve decision-making. The Indicators Portal features county-specific information from multiple sources, such as the U.S. Census Bureau, CDC and the Robert Wood Johnson Foundation. Seeger says within the next few months the site will include health indicators and data at both the city and county level.
“We want to make sure communities receive real, unbiased data that is understandable,” Seeger said. “The goal is that if a county government is looking at areas to improve health, the portal has all the information in one place to see what areas need improvement.”